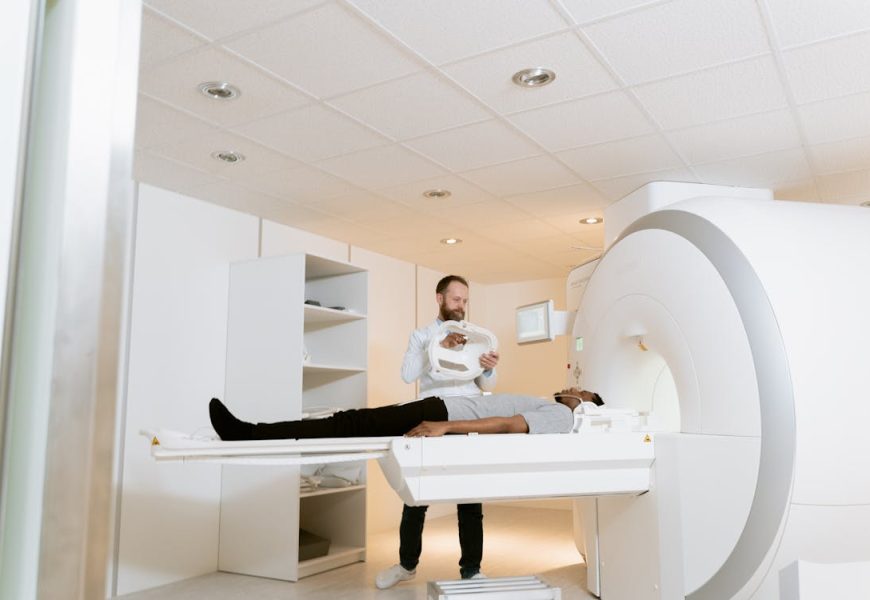
Artificial intelligence is changing how imaging centers work and how teams think about diagnostic care. Smart algorithms can speed image capture, improve image quality, and flag findings that might otherwise slip through the cracks.
Some of the newest platforms are built for real outpatient complexity, where varied case types, tight schedules, and diverse patient needs all intersect in a single day. These capabilities free up clinicians to focus on tricky cases and on patient contact rather than repetitive chores.
AI In Image Acquisition
Modern scanners paired with AI often adjust settings on the fly to fit a patient and the clinical question, so scans can be faster and gentler. Noise reduction and reconstruction methods that use machine learning can make low dose scans look sharper while preserving diagnostic detail in a wide range of body parts.
Technologists find that routine protocol tweaks become more consistent when the system suggests parameters based on prior scans and on simple feedback loops. That kind of automation cuts variability and helps radiology teams get more predictable quality from one shift to the next.
Intelligent Image Interpretation
Algorithms that analyze pixels can highlight areas that deserve a closer look and can sort cases so urgent reads come first on a list. These tools act like a second pair of eyes that never tires and that can mark subtle patterns across many images in short order.
Radiologists still carry responsibility for final calls, but they save time on routine reads and can focus their judgment where it matters most. Over time the group gains a shared mental model of when to trust machine output and when human instincts must take the lead.
Workflow Improvements For Staff
Scheduling, queuing, and report generation benefit when systems share timely status updates and simple alerts with front desk and clinical staff. Routine administrative steps that used to eat hours each day can be shortened with predictive schedules and clearer handoffs between teams.
Staff satisfaction often rises when repetitive tasks shrink and when people spend more time on patient contact and clinical problem solving. A practical rollout leaves room for feedback and tweaks so staff feel they helped shape how the tools fit daily routines.
Patient Experience And Access

When appointments are slotted with better estimates of how long each scan will take, waiting room stress goes down and patient flow improves. Clear explanation templates and visual guides driven by AI can help patients know what to expect without long phone calls or repeated instructions.
Faster turnaround on reports and on scheduling follow up scans means fewer phone tag episodes and less anxiety for patients and referring clinicians. Small gestures that save minutes at each step add up, and patients notice when the process runs smoother.
Quality Control And Risk Reduction
Automated checks can detect missing series, motion blur, or inconsistent contrast timing before a study is finalized, limiting wasted scans and repeat exposures. Audit logs and simple anomaly reports let managers spot patterns such as recurring scanner issues or training gaps that need attention.
When a machine flags a potential error, teams can review the case quickly and correct course so patient care stays steady. Over time these feedback loops reduce small mistakes and build confidence in both people and systems.
Operational Efficiency And Cost Control
Predictive maintenance models that watch scanner performance and alert staff to likely failures help avoid surprise downtime and costly last minute repairs. Scheduling that estimates case length with more nuance leads to fuller days without overbooking and to fewer rushed shifts that wear staff down.
Cost savings emerge from fewer repeats, lower waste, and from more efficient use of expensive imaging time. Leaders find that careful measurement of key metrics delivers clarity on where to invest next.
Data Management And Privacy
High quality labeled images are the fuel for many intelligent tools, so a plan for secure storage, consistent annotations, and curated archives matters more than ever. Privacy preserving techniques, such as models that train on local data and share only updates, let centers improve algorithms while keeping patient details guarded.
Clear retention policies and simple encryption practices help reduce exposure risk and keep legal teams calm. A pragmatic approach treats data as both an asset and a responsibility, with clear owners and simple rules.
Integration With Clinical Systems
When image analysis results flow smoothly into electronic health records and into order systems, clinicians get context without jumping between screens. Standards like DICOM and FHIR help glue systems together so that reports, alerts, and images remain linked to the same patient story.
Tight integration avoids duplicated work and reduces the chance that a critical result will sit in a silo. Teams that work across IT, clinical staff, and vendors usually find the best path forward through steady small improvements.
Training And Staff Adoption
Most teams trust a new tool after a few months of seeing reliable, measurable benefits and after leadership models the right way to use it. Hands on workshops, short micro learning modules, and shadow sessions let staff try features in a safe setting where mistakes are learning moments.
Early pilot projects that start small and expand based on lessons learned keep risk manageable and show quick wins that get people on board. When staff have a say in tweaks and workflows, uptake increases and the technology becomes part of daily craft rather than a black box.
Research And Continuous Improvement
Imaging centers that partner with academic groups or with local clinicians create useful feedback loops that test new models on real cases and that keep tools relevant to clinical needs. Continuous evaluation with clear metrics such as read time, repeat scan rate, and diagnostic concordance helps teams decide which models to keep and which to refine.
Simple governance with regular review meetings balances innovation energy with careful oversight so patient safety stays front and center. In practice the smartest programs treat model development as an ongoing conversation between clinicians, engineers, and operational staff.